Heart failure is a complex systemic condition of the heart that occurs due to the inability to maintain the supply to the demand required. This leads to improper and dysfunctional mechanical pumping of the heart, leading to morbidity and mortality. It may be due to structural or functional dysfunction, either during ventricular filling or ventricular ejection.
Based on the guidelines for the management of HF, the AHA/ACC/Heart Failure Society of America (HFSA) has classified HF into four main variations:
Heart failure with preserved ejection fraction (HFpEF)
Heart failure with reduced ejection fraction (HFrEF)
Heart failure with mildly reduced ejection fraction (HFmrEF), and
Heart failure with improved ejection fraction (HFimpEF)
Though pharmacological methods via Guideline-Directed Medical Therapy (GDMT) for improving heart function are the most common mode of management, non-pharmacological methods still play a vital role. This article dives into the importance of various non-pharmacological modifications in heart health management.
1. Lifestyle Modifications
Effective lifestyle modifications, adjunct to non-pharmacological methods, help reduce the burden of the disease. Heart failure is a multifactorial condition that requires comprehensive modifications.
1.1. Sodium Restriction
Increased salt retention by the kidney → Worsening of edema and congestion → Increased sympathetic activity → Peripheral vasoconstriction of afferent renal artery → Decreased blood flow to juxtaglomerular apparatus → Activates renin-angiotensin-aldosterone system (RAAS) → Angiotensin II and Aldosterone release → Sodium retention in proximal tubule and increased sodium reabsorption in distal tubules, respectively.
Though controversial, it is still recommended by The Korean Society of Heart Failure (KSHF), European Society of Cardiology (ESC), and American Heart Association/American College of Cardiology (AHA/ACC).
1.2. Fluid Restriction
A single-blind study carried out by Travers et al. investigated the clinical impact of fluid restriction; no significant difference was found in time to clinical stability, discontinuation of IV diuretic therapy, or stabilization of serum urea, serum creatinine, natriuretic peptides, or sodium in fluid-restricted patients.
Different guidelines recommend various approaches, including patient education after discharge from hospitalization, fluid restoration in severe heart failure, etc. However, fluid restriction is considered on a case-by-case basis.
1.3. Dietary Changes
Dietary changes are a great method, especially in cases with associated comorbidities of obesity or metabolic syndrome. A nutrition-deficient diet is recommended for overweight HF patients. Increased weight may contribute to increased cardiac load.
AHA/ACC guidelines recommend adherence to heart-healthy, evidence-based diets such as the Dietary Approaches to Stop Hypertension (DASH) diet, which focuses on reducing sodium intake while increasing consumption of fruits, vegetables, low-fat dairy products, and the Mediterranean diet.
Elderly HF patients should focus on household modifications along with diet modifications. Advanced HF (AHA/ACC stages C and D) with comorbidities may complicate treatment and require professional guidance and counseling.
1.4. Physical Activity
Physical activity increases quality of life, exercise capacity, and decreases hospitalizations. Exercise-based cardiac rehabilitation programs enhance functional status.
Current guidelines strongly recommend cardiac rehabilitation programs (CRP), including physical activity, risk factor and lifestyle modification, nutritional advice, psychological support, smoking cessation, regulation of body weight, and optimization of blood pressure for all eligible HF patients.
1.5. Weight Management
Weight loss has been associated with reduced risk of heart disease, while in patients with existing heart disease, the efficacy of weight loss is less clear. Though obesity has been linked with increased risk of HF, it has a protective effect in preexisting HF patients, while lower BMI has a higher risk of mortality. This phenomenon is called the “Obesity paradox.”
1.6. Substance Use Cessation

Alcohol, tobacco, cannabis, and cocaine use have been strongly linked with the onset and progression of HF. Tobacco usage increases the risk of coronary artery disease (CHD) along with other comorbidities.
1.7. Weight Monitoring and Education
Regular monitoring is crucial in detecting fluid retention, which indicates worsening HF. A sudden increase in weight (2 to 3 pounds per day/ 5 pounds in 1 week) indicates fluid overload and requires adjustment to medication regimen. Patient education regarding monitoring their own weight improves outcomes and leads to fewer HF exacerbations.
2. Advanced Interventions: Devices and Surgery
Cardiac resynchronization Therapy (CRT) and implantable cardioverter-defibrillators (ICDs) for selected patients with reduced ejection fraction to decrease mortality risk.
• Valve repair and coronary revascularization in appropriate clinical scenarios to improve outcomes when medical therapy alone is insufficient.
3. Management in Special Populations
It highlights the need for individualized care:
Elderly patients require adjustments for frailty, comorbidity burden, and polypharmacy.
• Women and sex-specific HF phenotypes (e.g., HF with preserved ejection fraction) demand tailored assessment and treatment strategies.
• Patients with comorbid conditions such as diabetes or chronic kidney disease benefit from integrated approaches that address overlapping pathophysiology.
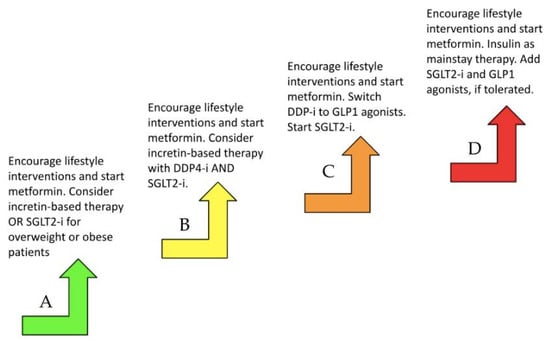
Thus, integrating lifestyle modification, advanced therapies, and personalized care frameworks into HF management can reduce morbidity, improve functional status, and extend survival, especially in vulnerable and special patient subgroups.
Reference:
Dugal, J. K., Malhi, A. S., Ramazani, N., Yee, B., DiCaro, M. V., & Lei, K. (2024). Non-Pharmacological Therapy in Heart Failure and Management of Heart Failure in Special Populations—A Review. Journal of Clinical Medicine, 13(22), 6993. https://doi.org/10.3390/jcm13226993




